
A global skin disease on the loose Efforts needed to eradicate leishmania in Yemen [Archives:2007/1040/Health]
April 9 2007
 |
 |
jamalnajar@hotmail.com
More than 350 million people are threatened by leishmania in 88 countries around the world, especially given that it's endemic in most developing countries. However, declaration of the disease is compulsory in only 32 countries, including Sudan, India and Saudi Arabia, whereas it's still neglected in more than 56 countries, which may lead to more victims and create numerous social problems, as it's one of the major enemies causing skin deformations.
Leishmania is a parasitic disease transmitted to humans by the bite of an insect vector called phlebotomine sandfly, which mainly lives in wet and dirty areas. Sandflies primarily become infected by feeding on animals; thus, when a female sandfly feeds on human blood, its painful sting injects the victim with the parasite.
Cutaneous, mucocutaneous and visceral are all forms of leishmania. With the third form considered fatal, the risk of the first and the second ones consists in skin deformity and other external parts due to lesions caused by the parasite.
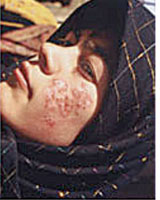
The disease's cutaneous form causes ulcers on exposed parts of the skin, such as the face, arms and legs. The disease produces lesions on these parts, often leaving its victims to lead a difficult social life due to anomalous skin scarring.
Mucocutaneous leishmania infects the mucous membranes of the nose, mouth and throat cavities, consequently causing serious deformations.
Leishmania's visceral form affects the internal parts of the body and can be characterized by swelling of the spleen and liver, irregular bouts of fever, substantial weight loss and anemia. The mortality rate for this form can be as high as 100 percent within two years if left untreated.
According to the World Health Organization, more than 12 million people are infected with leishmania, at approximately 2 million infections worldwide every year (1.5 million for cutaneous leishmaniasis and 500,000 visceral infections). The disease enjoys a wider distribution due to environmental and human-made factors.
The main risk factors related to cutaneous leishmaniasis are building dams and new irrigation schemes, which contribute to sandfly reproduction patterns in animal reservoirs. Concerning visceral leishmaniasis, irrigation plays a major role in disseminating the disease.
Additionally, wars, the proximity of homes to cowsheds and disruption of health services amplify the problem. Malnutrition also contributes to increasing the disease's severity, which increases due to weak immunity. Cracks and crevices in the walls of homes made of mud and dried grass provide shelter for sandflies, the main carriers of leishmania parasites.
Additionally, the spread of HIV infection brings about the severe visceral form of leishmania and increases the disease's epidemiology in dangerous ways. The two coexist in a deadly synergy, as HIV destroys the immune system; thus, the potential for visceral leishmania increases.
While leishmania threatens the lives of hundreds of thousands of Yemenis, especially children, cooperation between governments and organizations is required in order to eradicate the disease, which is endemic in several Yemeni governorates.
Visceral leishmania is the most common form in Yemen, whereas the other two forms are considered rare. Sandflies lives in valleys with flowing streams, such as Wadi Sardood, Hawaren, Lahima and Raija. Children are more subjected to the disease than adults, especially those between ages 1 and 7.
Leishmania is diagnosed by the parasite's demonstration in the aspirates of the spleen, bone marrow or lymph nodes. Because it's not a vaccine-preventable disease, its elimination is only possible via combat campaigns to provide infected individuals with medicine, in addition to educating them to be aware of the parasite's transmission circle.
However, numerous experiments and research have been conducted over the past 20 years in several countries in cooperation with international non-governmental organizations concerned with the disease in order to prepare a vaccine that can immunize people against leishmania parasites.
Islah Charitable Association recently called on international NGOs working in Yemen to support its combat efforts to eradicate the disease in Hodeidah, Hajjah, Sana'a, Raima and Mahwit governorates where the disease is widespread.
Dr. Isam Al-Din Awadh, director of the association's leishmania combat project, noted that he discussed with 25 international NGO representatives the association's combat efforts, as well as those of the Ministry of Public Health, which is conducting eradication campaigns in three governorates. Awadh's call came during a workshop organized by WHO in the United States a few weeks ago. He further mentioned that the association suggested to the workshop participants to hold a conference about the disease in Yemen to be attended by experts and international NGOs concerned with the disease. He added that Adrian Hopkins, director of the combat group, promised to adopt the suggestion and contact group members in order to prepare for the Yemeni conference.
According to the association's statistics, more than 282,000 citizens benefited from the leishmania combat project from 2001 to 2006.The project still is conducting field visits in the five targeted governorates, training volunteers in combat methods.
According to Dr. Qayed Ahmed Al-Haddad, head of Saba'een Hospital's pediatric emergency unit, the hospital receives approximately 10 leishmania patients per month, mostly from Raima, Taiz, Hodeidah and Amran governorates.
He explained that leishmania patients in Yemen face two major problems, the first of which relates to the scarcity of medicine to treat the disease. “Leishmania medicine is rare, but sometimes can be found with drug smugglers, in which case it costs between YR 20,000 and YR 30,000,” he noted.
The second problem relates to lack of coordination between NGOs concerned with the disease. “We sometimes receive cases urgently requiring immediate treatment because they arrive late from rural areas. However, we sometimes can't offer proper care to patients, so we transfer them to other hospitals. Direct cooperation between NGOs and hospitals is of vital importance in order to help patients who reach the hospital at severe risk,” Al-Haddad pointed out.
——
[archive-e:1040-v:14-y:2007-d:2007-04-09-p:health]


